Heit neurointerventional research lab
Stanford University
Our vision
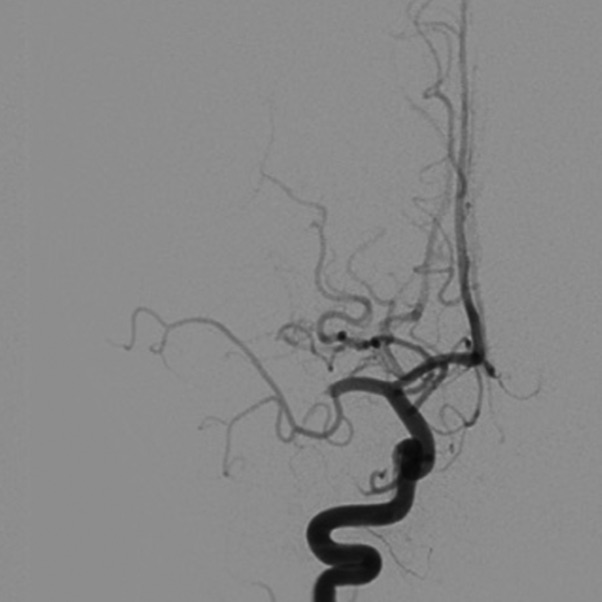
Our research seeks to advance our understanding of cerebrovascular disease and to develop new minimally invasive treatments for these diseases. We study ischemic and hemorrhagic stroke, cerebral aneurysms, delayed cerebral ischemia, cerebral arteriovenous malformations (AVMs), dural arteriovenous fistulae, and other vascular diseases of the brain. We use state-of-the-art neuroimaging techniques to non-invasively study these diseases, and we are developing future endovascular technologies to advance neurointerventional surgery.

Basic and Translational Science Research
From bench top...
Our basic and translational scientific team is working to advance our understanding of cerebrovascular development and patterning, the genetic basis of cerebrovascular malformation and aneurysm pathogenesis, and cellular adaption to cerebral ischemia. Our current knowledge about cerebrovascular development in humans is meager and limits our ability to develop new, molecularly targeted treatments for ischemic and hemorrhagic strokes. New knowledge about cerebrovascular development could generate new, molecularly targeted treatments for ischemic and hemorrhagic strokes and transform clinical paradigms for these diseases.

Clinical Research
...to bedside...
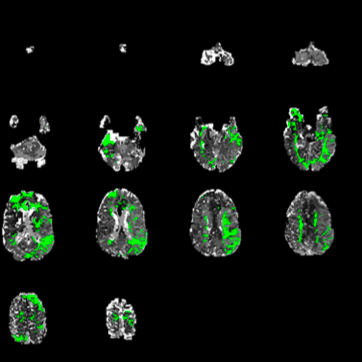
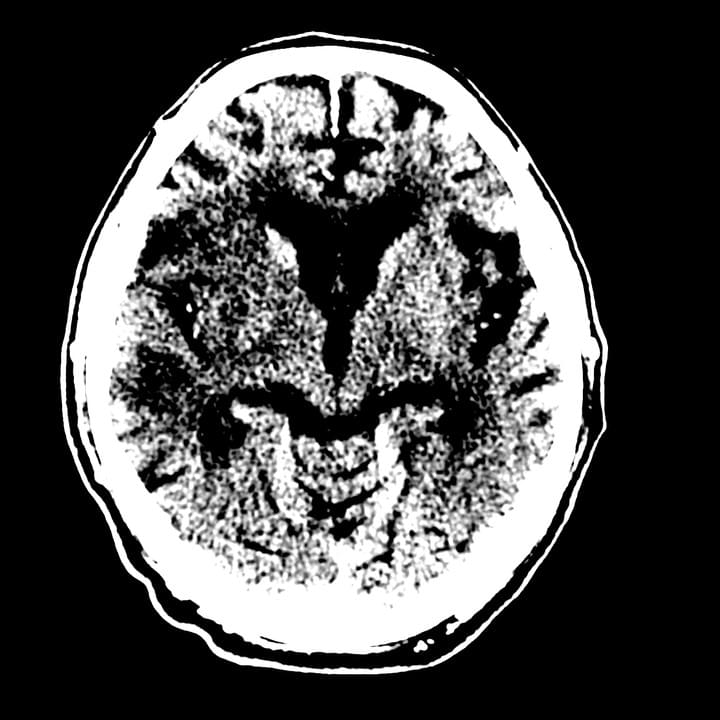
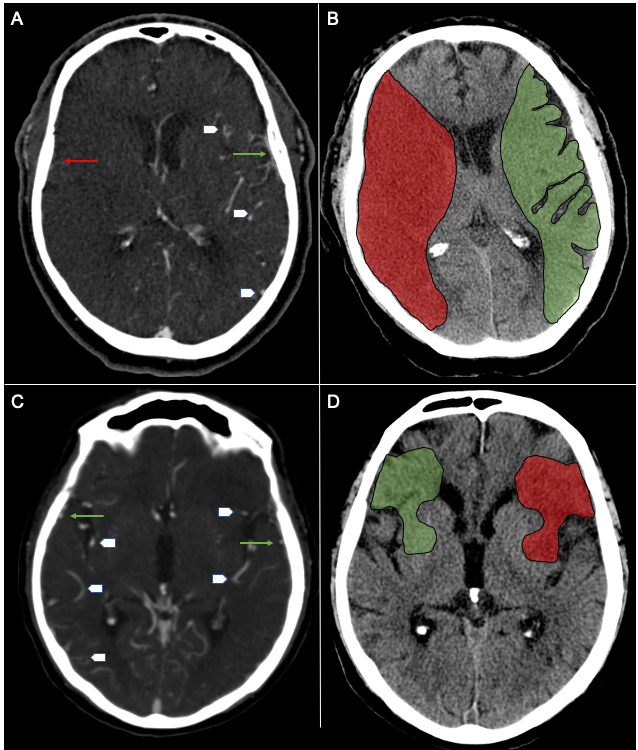
Our clinical research team seeks to advance our understanding of ischemic and hemorrhagic stroke pathophysiology and improve the non-invasive imaging evaluation and endovascular treatment of these diseases. In addition, we are working to identify circulating biomarkers of acute and subacute cerebral ischemia to identify patients at risk of stroke before it happens.

Development of Next Generation Stroke Devices and Therapies
...to patients
The Heit Lab partners with world-class engineers to develop the next generation of tools for the endovascular treatment of patients who suffer from strokes. Our team integrates clinical insight with cutting edge mechanical engineering to develop new endovascular devices and therpaies improve the treatment of stroke patients.
We recently undertook a wonderful collaboration with Renee Zhao, PhD's laboratory to develop the milli-spinner device for the treatment of patients with acute ischemic stroke. This device promises to vastly improve the removal of blood clots with a single thrombectomy attempt compared to current technology. You can read about the millspinner here.
We have also worked with a stellar engineering team led by Tania Moriomoto, PhD (UCSD) and Elliot Hawkes, PhD (UCSB) to develop a new catheter for the treatment of stroke patients. The catheter is called the VINE (Vascular Internal Navigation by Extension), which is a growing soft robot, a soft, which was inspired by climbing vines. The VINE catheter extends from its tip rather than sliding along the vessel wall, it imposes minimal friction and shear on the cerebrovascular endothelium, enabling atraumatic navigation of the tortuous and severely angulated anatomy that can prolong or defeat conventional catheter access. You can read about the VINE catheter here.
Together, these programs reflect our broader conviction that rigorous clinical science, paired with disciplined engineering, can produce fundamentally new paradigms of care for patients with acute ischemic stroke, hemorrhagic stroke, and other cerebrovascular diseases.The team
Our team comes from a variety of different backgrounds and has a wide range of expertise.

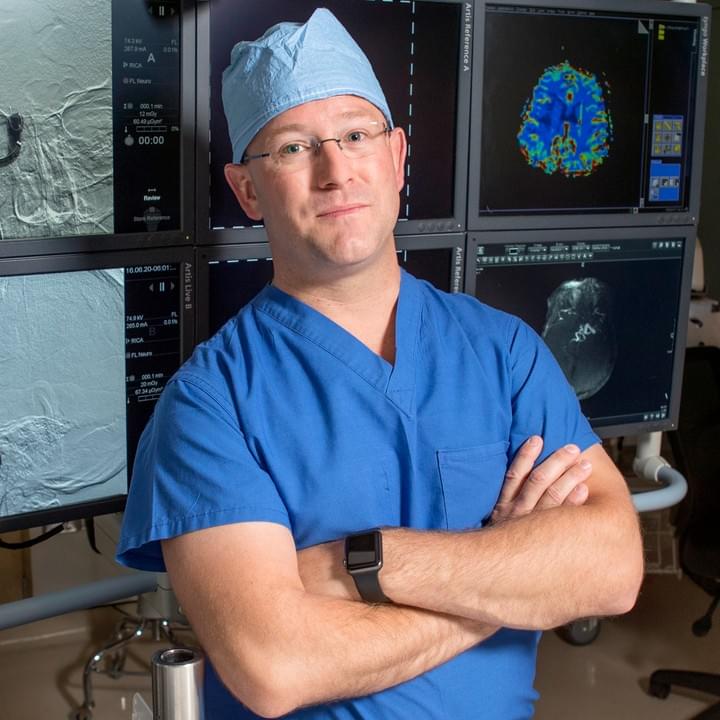
Jeremy J. Heit, MD, PhD
Principal Investigator
Dr. Heit is a Professor of Radiology and, by courtesy, of Neurosurgery at Stanford University. He is the Chief of Neuroimaging and Neurointervention (interim) at Stanford University, the Director of Neuroradiology at the Stanford Stroke Center, and the Director of the Stanford Neurointerventional Surgery Fellowship at Stanford.
His interest in research was piqued as an undergraduate student at the University of Colorado at Boulder, where he was a member of Tom Cech's lab. He completed his MD and PhD degrees at Stanford University, an internal medicine internship at the Brigham and Women's Hospital, a radiology residency at Massachusetts General Hospital, and a neurointerventional radiology fellowship at Stanford. He has been an attending neurointerventional surgeon and physician scientist at Stanford since 2015.

Henk van Voorst, MD, PhD
Postdoctoral Scholar
Dr. van Voorst received a BSc and MSc in Medicine from the Vrije Universiteit Amsterdam, an MSc in Information Studies: Track Data Science from the Universiteit van Amsterdam, and an MSc in Banking and Finance from the Universiteit Utrecht. He then obtained a PhD at the Amsterdam UMC, Universiteit van Amsterdam.
In his PhD studies, Dr. van Voorst focused on cost-effectiveness analyses and artificial intelligence in acute ischemic stroke imaging. In the Collaborations for New Treatments of Acute Stroke (CONTRAST) consortium, Dr. van Voorst was responsible for imaging data management and automated image analysis for several randomized clinical trials. In the Cost Effectiveness of CT Perfusion for Patients suffering from Acute Ischemic Stroke (CLEOPATRA) project, Dr. van Voorst was responsible for the model-based cost-effectiveness analyses.
Dr. van Voorst joined the Heit lab in September 2023. He received a Rubicon grant from the Dutch Scientific Council (NWO) for 24 months of postdoctoral training. Dr. van Voorst studies to possibilities of artificial intelligence-based artery and vein analyses in acute ischemic stroke imaging.

Pere Canals Canals, PhD
Postdoctoral Scholar
Dr. Pere Canals Canals is a Postdoctoral Scholar in the Department of Radiology at Stanford University, where he focuses on advancing medical imaging technologies with applications on vascular neuroradiology, with an emphasis on Stroke, under the mentorship of Dr. Jeremy Heit. Dr. Canals is an active recipient of the 2026 AHA Postdoctoral Fellowship, supporting his project GUIDE, where he is investigating how vision-language models can be leveraged in the context of acute stroke to improve speed and performance of diagnostic workflows in widely generalizable contexts. His research interests encompass medical image analysis, computer vision, deep learning, and 3D printing.
Dr. Canals earned his Ph.D. in Medicine at the Stroke Research group from the Vall d'Hebron Research Institute (VHIR) in Barcelona, Spain, under the leadership of Dr. Marc Ribó and co-supervised by Dr. Simone Balocco and Dr. Oliver Díaz, both researchers from the University of Barcelona (UB). Dr. Canals completed his doctoral studies between 2021 and 2024. His dissertation, titled "Arterial: an AI framework for the characterization of vascular tortuosity," received the highest distinction of Cum Laude. For his Ph.D., he was awarded the PERIS PIF-Salut doctoral grant by the Catalan Health Department. Moreover, he led funding acquisition and development of the "Arterial" project, securing €107,690 in funding from the Spanish Health Institute to support his research.
Prior to his doctoral studies, Dr. Canals completed a Bachelor of Science in Engineering Physics at the Universitat Politècnica de Catalunya (UPC) in Barcelona. He conducted his bachelor's thesis at the Technion - Israel Institute of Technology in Haifa, focusing on astrophysics and stellar population simulations. He then pursued a Master of Science in Biomedical Engineering at the University of Barcelona (UB), during which he participated in an exchange program at TU Delft in the Netherlands, where he was introduced to the field of deep learning. Notably, Dr. Canals achieved top 1% rankings in the Catalonia and Spain university entrance exams, earning him a prize from the Fundació Catalunya-La Pedrera.
Alexander Salerno, MD, PhD
Postdoctoral Scholar
Dr. Alexander Salerno is a Postdoctoral Scholar in the Department of Radiology at Stanford University. As a neurologist and stroke specialist, he is dedicated to advancing neuroimaging technologies and directly improving clinical care for patients with cerebrovascular disease. His research in the Heit Lab focuses on the clinical and radiological evaluation of patients with acute ischemic stroke, with a special emphasis on posterior circulation stroke management. He will develop pipelines that refine prognostic models using multimodal imaging to help guide acute treatment decisions.Dr. Salerno earned his MD at the University of Genoa, Italy, followed by his neurology residency, an MD-PhD in cerebrovascular disease, and a postdoctoral fellowship at the Stroke Center of Lausanne University Hospital in Switzerland. At Lausanne, he also holds a faculty appointment as Reader and Clinical Faculty (MERc-PD). An effective catalyst for collaborative research with a strong clinical research background, he actively coordinates international multicenter collaborations and helps establish large-scale, federated data-sharing networks for international stroke registries. Alongside his research, he is dedicated to medical education and enjoys finding engaging ways to teach clinical neurology.
Fun fact: when he is not analyzing brain scans or asking patients to repeat "No ifs, ands, or buts," Alexander is a passionate marine aquarist who loves aquascaping miniature coral reefs right in his living room. An avid traveler with a creative eye for designing scientific illustrations, he also enjoys unwinding by cooking authentic Italian cuisine.

Simon Levinson, MD
Resident, Neurosurgery
Simon is a PGY - VI neurosurgery resident at Stanford and a research associate in the Heit lab. He is training to become a dual trained open and endovascular neurosurgeon and will be a neurointerventional fellow at Stanford after completion of his surgical training. He completed his undergraduate studies at UCLA in Los Angeles where he earned a BA in political philosophy with a minor in neuroscience and remained at UCLA where he graduated from the David Geffen School of Medicine in 2021.
Simon is passionate about finding new ways to help patients recover from neurologic injury and his work in the Heit lab focuses on basic science and translational therapies for patients recovering from acute strokes. He is currently working to investigate the immunologic mechanism that could influence how patients recover after experiencing a stroke with the ultimate goal of developing neuro protective therapies that improve patient outcomes.

Samantha Rhodes, BS
Research Assistant
Sam Rhodes is a research assistant in the Department of Radiology and the Heit Lab. She grew up in the Chicago area, and she attended the University of California at Davis for college. While at UC Davis, she swam as a division I athlete for four years, and she majored in Neurobiology, Physiology, and Behavior. Following her graduation from UC Davis, she joined the Heit Lab, where she is studying the imaging evaluation and minimally invasive treatment of patients with acute ischemic stroke. She also serves as a member of the Stanford Stroke Center clinical coordinator team.

Anna Maria Bombardieri, MD, PhD
Faculty Research Collaborator
Dr. Bombardieri is and Assistant Professor in the Department of Anesthesiology at Stanford and a faculty research collaborator in the Heit Lab. She earned her medical degree from the University of Rome, La Sapienza, and completed her residency training and PhD at the University of Florence. Subsequently, she pursued fellowships in Regional Anesthesia and Acute Pain Medicine at the Hospital for Special Surgery in New York, followed by a Critical Care Medicine fellowship at the Free University of Brussels.
In the Heit Lab, her research centers on developing a neuroimaging perfusion score to detect of cerebral vasospasm and exploring minimally invasive techniques to treat patients suffering from vasospasm following aneurysmal subarachnoid hemorrhage.
Her ultimate goal is to utilize minimally invasive regional anesthetic techniques to enhance neurological outcomes in stroke patients.
Alumni
Graduates of the Heit lab continue to do amazing things!

Eric Sussman, MD
Associate Professor, University of Connecticut
Dr. Sussman is a neurosurgeon with Hartford Healthcare. He was a prior Neurosurgery Resident, Neurointerventional Surgery Fellow at Stanford and a Research Associate in the Heit Lab. Dr. Sussman completed his undergraduate degree at Duke University and his MD at the Icahn School of Medicine at Mount Sinai in New York. Dr. Sussman's research in the Heit lab focused on the identification of factors that predict clinical outcomes following ischemic and hemorrhagic stroke as well as neurovascular proteomics and metabolomics.

Tobias Faizy, MD
Professor, Munster University, Germany
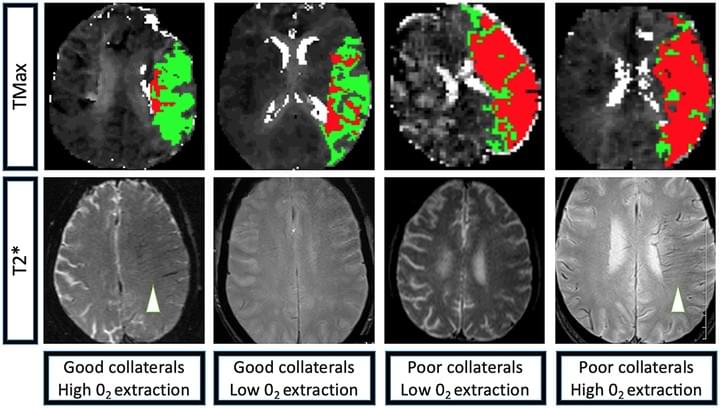
Dr. Faizy is Professor of Neuroradiology at Munster, Germany. During his postdoctoral studies in the Heit Lab, Dr. Faizy worked to understand better how collateral blood flow maintains brain tissue viability during ischemic stroke. His innovative contributions led to publications in Stroke, Radiology, the Journal of Cerebral Blood Flow and Metabolism, and other prestigious journals. Dr. Faizy continues to collaborate with Dr. Heit from "across the pond."

Reza Kabiri, BS
MD/PhD Student, University Medical Center, Hamburg-Eppendorf
Mr. Kabiri is a MD PhD student in Hamburg, Germany, and he was a research associate at Stanford University during his time in the Heit Lab. His research interests include stroke imaging, artificial intelligence, and advance imaging of cerebral ischemia.

Matt Leipzig, BS
Research Associate
Mr. Leipzig is currently working as an artificial intelligence consultant. During his time as a research associate in the Heit Lab, he worked to develop statistical models that can improve both prediction and inference related to stroke. He also performed machine learning analyses to advance our understanding of ischemic and hemorrhage stroke.

David Marcellus, BS
Clinical Research Coordinator
Mr. Marcellus is a Clinical Research Coordinator at Stanford University and a Heit Lab alumni. He graduated from Cal Poly San Luis Obispo and joined Heit Lab as a Research Associate. After one year in the Heit Lab, he transitioned to a Clinical Research Coordinator, where he currently works. He continues to collaborate with Dr. Heit and serves as the clinical research efforts of the Heit Lab and the Stanford Neurointerventional Radiology service.

Shruti Arora, BS
Life Science Research Professional
Ms. Arora is a MD/PhD student at the University of California at Davis. She was previously a LSRP in the Heit Lab, and her research with Dr. Heit focused on murine models of acute ischemic stroke. She also performed cutting edge brain microscopy imaging using CLARITY to study developmental cerebral vasculature patterning and vascular changes during ischemic stroke.

Dylan Wolman, MD
Neurointerventional Surgery Fellow and Research Associate
Dr. Wolman was previously a Radiology Resident and Neurointerventional Fellow at Stanford and a Research Associate in the Heit Lab. Dr. Wolman completed his undergraduate degree at Brandeis University and his MD at Tufts University School of Medicine. Dr. Wolman completed his Neurointerventional Surgery Fellowship at Stanford in 2020 after completion of his radiology residency. In the Heit Lab, Dr. Wolman's research focused on novel imaging techniques, such as dual energy CT and perfusion imaging, for the evaluation of acute ischemic stroke.
He is currenlty an Assistant Professor of Radiology at Brown University.

Gabriella Kuraitis, BS
Research Assistant
Ms. Kuraitis is a prior research assistant in the Heit Lab. She completed her undergraduate degree in the biological sciences with an emphasis on neuroscience at the University of Oregon. She has had prior research experience at Stanford University and University of California, San Diego, which included a study to determine if artificial intelligence could be used to screen patients with retinal diseases. Her research interests in the Heit Lab are focused on stroke imaging and predicting clinical outcomes of ischemic and hemorrhagic strokes.

Sophie Ostmeier, MD
Postdoctoral Student
Dr. Ostemeier is a former r post doc in the Heit Lab. She completed her MD at the Technical University of Munich. Before being recruited to Dr. Heit's lab at Stanford, she studied dual energy CT applications in radiology. Her research interests focus on developing artificial intelligence techniques for the evaluation of cerebral ischemia and hemorrhagic stroke. She is an avid runner and cyclist, and she enjoys climbing the hills overlooking the Stanford campus and Bay Area in her free time.
She is currently a radiology resident in Germany.

Sarah Snyder, BA
Research Associate
Sarah Snyder is was a clinical research assistant in the Department of Neurosurgery at Massachusetts General Hospital and a pior research associate in the Heit Lab. She completed her BA at the Duke University. Sarah is an accomplished swimmer, and she was Captain of the Duke Swim Team and an Olympic Trials qualifier.
In the Heit Lab, Sarah studied cerebral aneurysms and the morphologic assessment of aneurysms using artificial intelligence platforms.
She is currently a medical student at Temple University in Philadelphia, PA

Gautam Adusumilli, MD
Research Assistant
Dr. Adusumilli is Research Associate in the Heit Lab and a PGY-1 Surgery resident at Stanford. He discovered Neurointerventional Surgery while completing his BA and MD degrees at Washington University in St. Louis. His research in the Heit Lab focuses on novel measures of collateral blood flow in ischemic stroke patients, such as venous outflow. His long-term aspiration is to translate endovascular techniques to low-resource environments. Dr. Adusumilli will enter a Radiology Residency at Massachusetts General Hospital in 2022, and he will continue to collaborate with Dr. Heit after he moves to Boston.

Aroosa Zamarud, MD
Postdoctoral Scholar
Dr. Zamarud completed her undergraduate education at Bannu Medical College, Khyber Medical University, Pakistan. She then worked serving underprivileged communities in remote vilages of northern Pakistan.
In March 2022, Dr. Zamarud joined Stanford Neurosurgery department as a Visiting Instructor with Dr. Steve Chang's research group. She studied neuro-oncology, with a special emphasis on exploring the potential of Cyberknife stereotactic radiosurgery for various brain pathologies.
Dr. Zamarud was then recruited to the Heit Lab, where she is currently a postdoctoral fellow. While in the Heit Lab, she studied venous outflow in patients with acute ischemic stroke and hemorrhagic stroke.
She is currently a surgical intern at Einstein University in New York City, NY.

Adrien Guenego, MD
Faculty Research Collaborator
Dr. Guenego is a neurointerventional radiologist at Erasme Medical Center in Brussels, Belgium. He was previously a Research Fellow and Visiting Scholar at Stanford, both in the Stanford Stroke Center and in the Heit Lab. Dr. Guenego continues to work with Dr. Heit on research topics based in neurointerventional radiology.
Dr. Guenego completed his undergraduate degree at Toulouse University in France. His MD was also completed in France at Toulouse University Hospital, and Fondation Rothschild in Paris as well as at CHUV in Lausanne, Switzerland. Dr. Guenego then completed a Neurointerventional Surgery Fellowship in Brussels from 2020-2022. He now practices at the prestigious Erasme Medical Center while he completes his PhD at Brussels University that if focused on vasospasm and delayed cerebral ischemia after cerebral aneurysm rupture.
Dr. Guenego continues to study cerebrovascular disease and neurointerventional devices and techniques for the treatment of these diseases in collaboration with Dr. Heit. In addition, he has a strong interest in entrepreneurship and is working on scaling-up two health companies.

Jamie Kesten, BS
Research Assistant
Jamie Kesten is a prior research assistant in the Heit Lab. She was born at Stanford Hospital and grew up in the area. She completed her undergraduate studies at Vassar College, where she majored in Neuroscience and French. At Vassar, she played on the volleyball team, served as a tour guide, and interned in the Department of Philosophy. After graduation, Jamie joined the Heit Lab, where her research is focused on the imaging and treatment of patients with acute ischemic stroke, neuroinflammation, artificial intelligence, and spine procedures. She is an aspiring physician, and she hopes to treat pediatric patients in the future.
She is currently a medical student at the University of California at Irvine.

Maya Schwartz, BA
Research Assistant
Maya Schwartz is a prior research assistant in the Heit Lab. She grew up in the San Francisco bay area, and she completed her BA in Neuroscience and Spanish at Middlebury College, where she graduated Summa Cum Laude. After graduating from Middlebury, she joined the Heit Lab as a research assistant, and her research focused on the imaging evaluation of patients with acute ischemic stroke. She authored two first author papers and several other manuscripts during her time in Heit Lab.
She is currently a medical student at the University of Michigan.
News and press
Read more...Congratulations to Dylan Wolman, MD for winning the Adult Brain Outstanding Presentation Award at...April 22, 2020Read more...Congratulations to Dr. Faizy for being awarded the 2020 German Research Foundation Grant to...Read more...Congratulations to Dr. Sussman for being awarded the competitive Joe Niekro Foundation Research...Read more...Congratulations to Dr. Wolman for being awarded the prestigious RSNA Research Resident Grant for...April 25, 2019Read more...Congratulations to Dr. Faizy for being awarded the 2019 German Research Foundation Grant to...Publications
Selected publications from the Heit Lab

Comprehensive List of Dr. Heit's Publications
Pubmed Bibliography

Perfusion Imaging Predicts Favorable Outcomes After Basilar Artery Thrombectomy
Cereda C, et al. (2021) Annals Neurology Nov 17. doi: 10.1002/ana.26272

Distinct intra-arterial clot localization affects tissue-level collaterals and venous outflow profiles
Faizy TD, et al. (2021) European Journal of Neurology. Dec;28(12):4109-4116. doi: 10.1111/ene.15079. Epub 2021 Aug 30.

Reperfusion Therapies for Children With Arterial Ischemic Stroke
Heit JJ, et al. (2021) Topics in MRI. Oct 1;30(5):231-243.
doi: 10.1097/RMR.0000000000000273.

VINE Catheter for Endovascular Surgery
Li M, et al. (2021) IEE Transactions on Medical Robotics and Bionics 3: 384-391

MR perfusion imaging: Half-dose gadolinium is half the quality
Heit JJ, et al. (2021) J Neuroimaging May 18. doi: 10.1111/jon.12879.

Assistance from Automated ASPECTS Software Improves Reader Performance
Delio PR, et al. (2021) J Stroke Cerebrovascular Dis May 10;30(7):105829.
doi: 10.1016/j.jstrokecerebrovasdis.2021.105829.

Association of Venous Outflow Profiles and Successful Reperfusion After Thrombectomy
Faizy TD, et al. (2021) Neurology May 5;10.1212/WNL.0000000000012106.
doi: 10.1212/WNL.0000000000012106

Computed Tomography-Based Imaging Algorithms for Patient Selection in Acute Ischemic Stroke
Pulli B, Heit JJ, and Wintermark M (2021) Neuroimaging Clin N Amer May;31(2):235-250. doi: 10.1016/j.nic.2020.12.002.Epub 2021 Mar 23.

Venous Outflow Profiles Are Linked to Cerebral Edema Formation at Noncontrast Head CT after Treatment in Acute Ischemic Stroke Regardless of Collateral Vessel Status at CT Angiography
Faizy T, et al. (2021) Radiology Apr 6;203651. doi: 10.1148/radiol.2021203651. Online ahead of print.

Non-contrast dual-energy CT virtual ischemia maps accurately estimate ischemic core size in large-vessel occlusive stroke
Wolman DN, et al. (2021) Scientific Reports Mar 24;11(1):6745. doi: 10.1038/s41598-021-85143-3.

Favorable Venous Outflow Profiles Correlate With Favorable Tissue-Level Collaterals and Clinical Outcome
Faizy T, et al. (2021) Stroke Mar 8;STROKEAHA120032242.
doi: 10.1161/STROKEAHA.120.032242.Online ahead of print.

Perfusion imaging-based tissue-level collaterals predict ischemic lesion net water uptake in patients with acute ischemic stroke and large vessel occlusion
Faizy T, et al. (2021) JCBFM Feb 8;271678X21992200. doi: 10.1177/0271678X21992200.

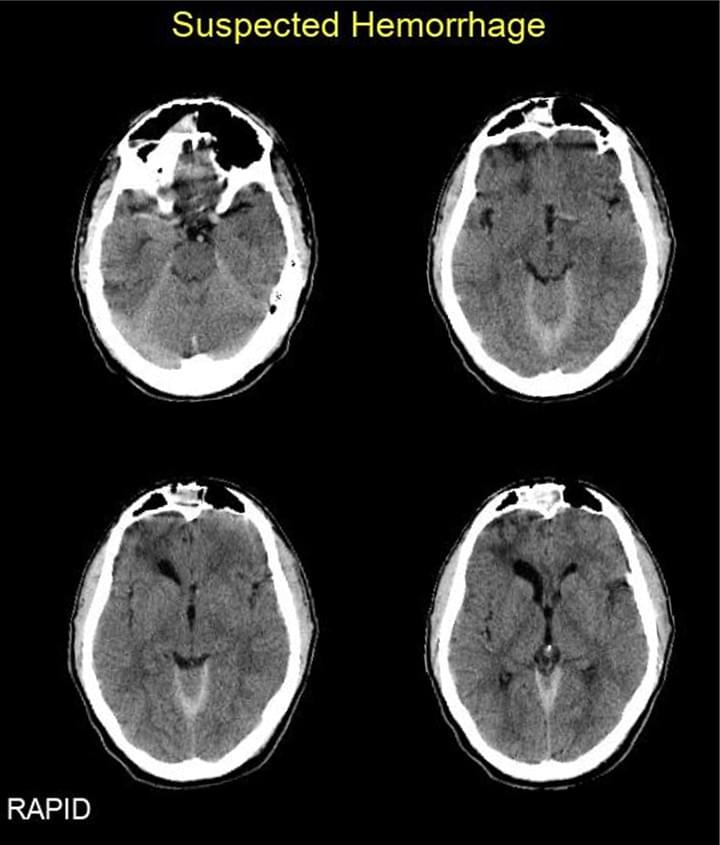
Automated Cerebral Hemorrhage Detection Using RAPID
Heit JJ, et al. (2021) AJNR Jan;42(2):273-278. doi: 10.3174/ajnr.A6926. Epub 2020 Dec 24.

High-Performance Automated Anterior Circulation CT Angiographic Clot Detection in Acute Stroke: A Multireader Comparison
Dehkharghani S, et al. (2021) Radiology Mar;298(3):665-670. doi: 10.1148/radiol.2021202734. Epub 2021 Jan 12.

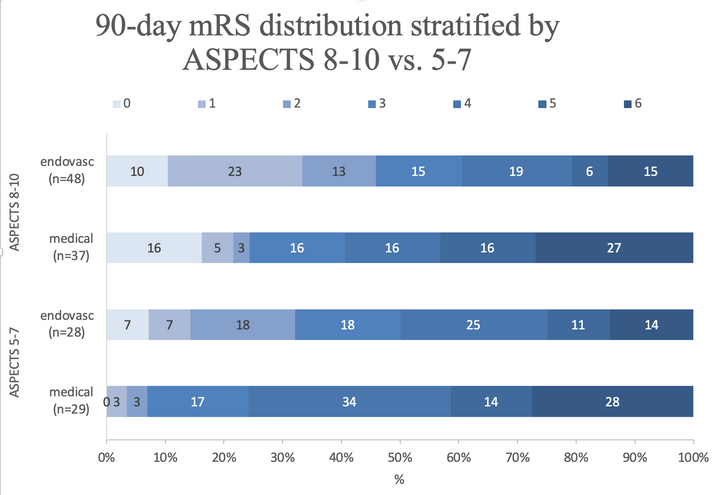
CT perfusion core and ASPECT score prediction of outcomes in DEFUSE 3
Kim-Tenser M, et al. (2020) Int J Stroke Mar 31;1747493020915141. doi: 10.1177/1747493020915141.
https://pubmed.ncbi.nlm.nih.gov/32233746/https://pubmed.ncbi.nlm.nih.gov/32233746/

Effect of Oxygen Extraction (Brush-Sign) on Baseline Core Infarct Depends on Collaterals (HIR)
Guenego A, et al. (2021) Front Neurol Jan 6;11:618765. doi: 10.3389/fneur.2020.618765. eCollection 2020.

Thrombectomy for acute ischemic stroke in nonagenarians compared with octogenarians.
Sussman ES, Martin B, Mlynash M, Marks MP, Marcellus D, Albers G, Lansberg M, Dodd R, Do HM, Heit JJ. (2020) Thrombectomy for Acute Ischemic Stroke in Nonagenarians Compared to Octogenarians. JNIS 12:266-270.

Endovascular versus medical therapy for large-vessel anterior occlusive stroke presenting with mild symptoms.
Wolman DN, et al. (2019) Int J Stroke. doi: 10.1177/1747493019873510

Rapid Neurologic Improvement Predicts Favorable Outcome 90 Days After Thrombectomy in the DEFUSE 3 Study
Heit JJ, et al. (2019) Stroke. May;50(5):1172-1177. doi: 10.1161/STROKEAHA.119.024928

Collateral blood flow measurement with intravoxel incoherent motion perfusion imaging in hyperacute brain stroke.
Federau C, et al. (2019) Neurology. May 21;92(21):e2462-e2471. doi: 10.1212/WNL.0000000000007538

Hypoperfusion Intensity Ratio Is Correlated With Patient Eligibility for Thrombectomy.
Guenego A, et al. (2019) Stroke. Apr;50(4):917-922. doi: 10.1161/STROKEAHA.118.024134
join the heit lab team
Submit a CV and a brief description of your research interests and career goals to Jeremy Heit, MD, PhD at jheit@stanford.edu
Post Doctoral Candidates - Basic/Translational Science Research Group
We are looking for qualified post doctoral candidates to join our group. Applicants to the basic science/translational research team should have an interest in advancing our understanding of cerebrovascular developmental biology and patterning, ischemic stroke physiologic imaging and treatment in animal models, nano-therapeutic treatment of ischemic stroke or delayed cerebral ischemia after cerebral aneurysm rupture, or novel interests pertinent to the field of neurointerventional surgery. Candidates must hold a PhD or MD from an accredited institution and have excellent laboratory and analytical skills. Independence and critical thinking are highly valued skills.
Post Doctoral Candidates - Clinical Science Research Group
We are looking for qualified post doctoral candidates to join our group. Applicants to the clinical research team should have an interest in ischemic and hemorrhagic stroke pathophysiology and the non-invasive imaging evaluation and endovascular treatment of these diseases. We are particularly interested in how the brain adapts to cerebral ischemia to maintain neurologic function in the setting of severe cerebral blood flow compromise. Candidates must hold a PhD or MD from an accredited institution and have excellent analytic skills. Computational, programming, independence, and critical thinking are highly valued skills.
Research Associate - Clinical or Basic/Translational Science Research Groups
Looking to gain research experience or learn more about cerebrovascular disease and its cutting-edge treatment? We are looking for qualified research associate candidates to join our group. Applicants should have a Bachelor's degree from an accredited institution and an interest in cerebrovascular disease. Candidates with an interest in pursuing clinical medicine or research are encouraged to apply. Independence, and critical thinking are highly valued skills.
Support Our Research
A gift to the Heit Lab will support our cerebrovascular disease and neurointerventional treatment research.
If you would like to make a donation for this purpose, please contact:Erik C. Rausch
Stanford Medical Center Development
Phone: 650-725-1005
Email: erausch@stanford.edu
Online gifts can also be made here: https://medicalgiving.stanford.edu
Contact us
Jeremy J. Heit, MD, PhD - Academic Office
Department of Radiology and, by courtesy, of Neurosurgery
Center for Academic Medicine
Department of Radiology 5659-324A
453 Quarry Road
Palo Alto, CA 94304
jheit@stanford.edu
Dr. Heit's Clinic - Patient Care
Stanford Neuroscience Health Center
213 Quarry Rd
Palo Alto, CA 94304
(650) 723-6469 (Clinical Appointments)
Jeremy J. Heit, MD, PhD Stanford Faculty Profile
© 2019 by Jeremy Heit, MD, PhD